In the world of medical science, the most innovative ideas often come from the most unexpected sources. For the UC Berkeley Professor of Bioengineering, Dr. Phillip Messersmith, inspiration strikes from mussels. By studying the adhesive properties of these sea creatures, Messersmith hopes to create a bio-inspired ‘glue’ that can seal delicate fetal membranes post surgery.
On wet and stormy coastlines, survival for sea creatures like mussels, oysters, and barnacles depends largely on their ability to stay put despite the oceanic currents. Luckily, over the past 100 million years (a rather long evolutionary timeline), mussels have mastered this skill. Mussels construct byssal threads, known as their “beard,” to secure themselves to rocks and each other. These threads are formed when microscopic glands within the foot secrete special proteins which fuse together to create the core of the thread. Additional proteins surround the core, fortifying the thread’s strength and tenacity.
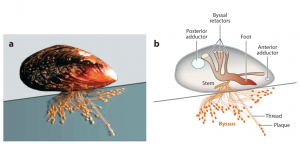
The byssal threads secreted by the mussel’s foot help hold the mussel in place in harsh oceanic conditions.
Dr. Messersmith’s journey into this remarkable research began with his realization that the oceanic environment where the mussel subsides and the watery environment inside the amniotic sac, where the fetus develops, are quite similar.
Fetal surgery, which is used to correct anatomical defects while the fetus is still in the uterus, addresses life threatening conditions like spina bifida—a rare lower neural tract defect causing approximately 1 in 2,700 newborns to be delivered with the spinal cord exposed. Another high-risk condition that often calls for fetal surgery is twin-twin transfusion syndrome (TTTS). In this scenario, twins share a single placenta, resulting in uneven blood flow between the two siblings. Surgeons often use fiber optics to cauterize the blood exchange and give both twins a fighting chance at life.
In any fetal surgical procedure, an underlying concern remains: once punctured, the fetal membrane does not heal. It is difficult to suture or staple it closed and there are currently no FDA-approved sealants and adhesives. The unsealed membrane puts the fetus at high risk of premature labor. With each week passing before the 28 week gestation period, the babies’ chances of surviving preterm delivery decrease exponentially. If the baby is born before 23 weeks, there is a less than 10 percent chance of survival. If the baby is delivered, there is also a high risk of severe disability including impairments in brain development and retinopathy.
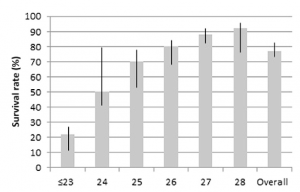
Survival rates according to gestational age (GA) among 1718 very low birth weight infants of GA 28 weeks admitted to five training centers for the Premature Baby Foundation of Taiwan from 2007 to 2012. The thin lines indicate ranges across centers.
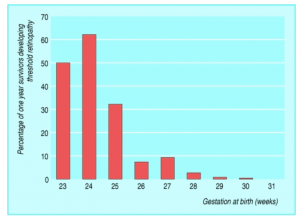
Risk of retinopathy among survivors tends to increase as the baby is born earlier. Image courtesy of Michael Colvin
Dr. Messersmith’s research gives hope to this dire situation. In mussels, L-dopa is one of the amino acids added to the byssal threads to increase adhesion. In humans, L-dopa is not a common protein building block but is instead a precursor to dopamine, the neurotransmitter responsible for feelings of happiness. Through experiments on human fetal membrane tissue, Dr. Messersmith showed that L-dopa can be used to seal membrane tissue post surgery.
Further experimentation on rabbits showed that when L-dopa amino acids are linked together via a peptide bond and chemically cross-linked, the L-dopa polymers can increase the survival rate for bunnies with a punctured fetal membrane to 80%, a dramatic improvement from a 35% survival rate in the control.
A recent collaboration with doctors from the University Hospital at Zurich is accelerating progress on this project, making clinical application a soon-to-be reality. The team of researchers designed an umbrella applicator device that could be implanted into the fetal membrane via a trocar puncture, a technique using a pen-shaped instrument with a sharp triangular point at one end to create an opening during surgery. While the effectiveness of this applicator device is currently being tested on sheep, early results are brimming with promise.
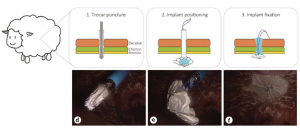
The umbrella applicator device being implanted via trocar puncture into a fetal membrane. Image courtesy of Devaud et al.
For example, it should be possible for the materials to be delivered via a minimally invasive surgical approach. Since these materials will be in direct contact with fetal organs, they must be compatible with the cell climate. They should also be flexible enough to accommodate the fetus’s growth throughout pregnancy and be impenetrable to external fluids. The long-term effects of the implanted materials need to be researched before clinical implementation.
Although many questions still need to be answered, Dr. Messersmith’s innovative research fusing nature’s wisdom and human ingenuity can enable fetal surgery to help more families deliver healthy children.
Works Cited:
Messersmith Lab» Bioinspired Materials Research at UC Berkeley. (2020). Berkeley.edu. https://bioinspiredmaterials.berkeley.edu/
Winkler, S. M., Harrison, M. R., & Messersmith, P. B. (2019). Biomaterials in fetal surgery. Biomaterials Science, 7(8), 3092–3109. https://doi.org/10.1039/c9bm00177h
Mighty Mussels Have Industrial Strength. (2010, March 5). NPR. https://www.npr.org/2010/03/05/124319594/mighty-mussels-have-industrial-strength
Colvin, M. A., McGuire, W., & Fowlie, P. W. (2004). Neurodevelopmental outcomes after preterm birth. BMJ, 329(7479), 1390–1393. https://doi.org/10.1136/bmj.329.7479.1390
Laparoscopic Trocars Provide Access Points for Surgery | Laparoscopic.MD. (2023). Laparoscopic.md. https://www.laparoscopic.md/surgery/instruments/trocar#:~:text=In%20its%20simplest%20form%2C%20a,an%20access%20port%20during%20surgery.
Devaud, Y. R., Senta Stäuble, Ueli Moehrlen, Weisskopf, M., Ladina Vonzun, Zimmermann, R., Ehrbar, M., & Ochsenbein‐Kölble, N. (2021). Minimally Invasive Precise Application of Bioadhesives to Prevent IPPROM on a Pregnant Sheep Model. Fetal Diagnosis and Therapy, 48(11-12), 785–793. https://doi.org/10.1159/000519910
